If you’ve been battling “stubborn acne” with every salicylic acid wash in the aisle only to find it gets redder, itchier, and more persistent, I have a secret for you: it might not be acne at all. In 2026, a landmark study by the Global Skin Microbiome Initiative revealed that nearly 18% of adult “acne” cases are actually an overgrowth of yeast, not bacteria. Welcome to the world of Malassezia folliculitis.
This isn’t your standard breakout. It’s a microbiome imbalance that requires a specialized fungal acne treatment plan. Whether you are looking for a professional dermatologist’s fix or a fungal acne treatment at home, this guide will help you stop “feeding the fungus” and start healing your skin barrier for good.
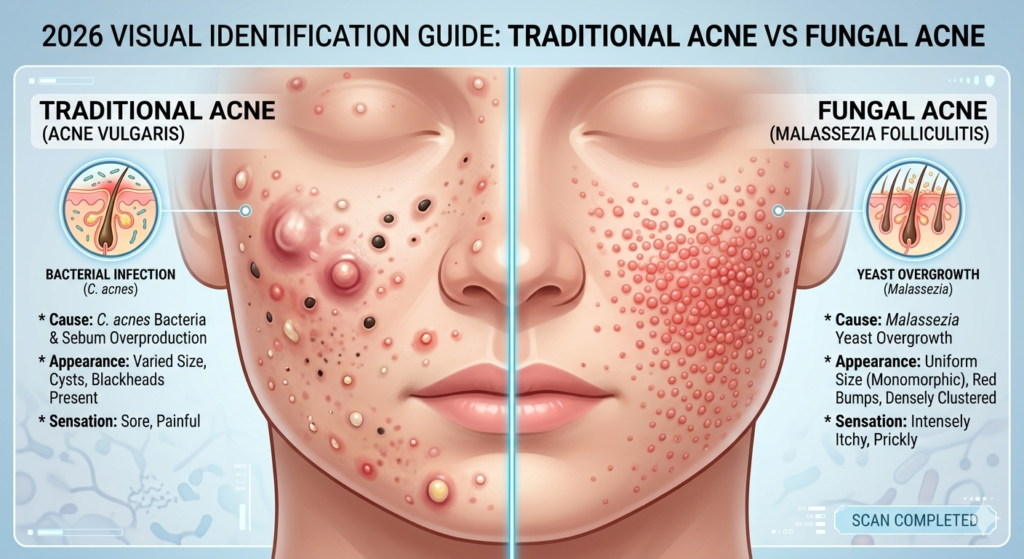
1. Identification: Is Your Breakout Actually Fungal?
Before we talk about how to get rid of fungal acne, we have to identify it. Standard acne treatments like Benzoyl Peroxide often fail here because they don’t target yeast.
The “Fungal” Checklist:
- The Itch Factor: Does your skin crawl or itch when you sweat? 82% of sufferers report a “prickly” sensation, a major red flag for fungal acne treatment.
- Uniform Appearance: Are the bumps all the same size? Yeast colonies tend to be “monomorphic”—identical 1-2mm red bumps.
- Temperature Sensitivity: Does it flare up the moment the temperature hits 30°C (86°F) or humidity exceeds 70%?
- Real User Experience: “I thought it was just bad summer breakouts, but the constant itching on my forehead was driving me crazy. Once I stopped my oily moisturizer, the ‘crawling’ feeling stopped in 48 hours.” — Sarah, 29, Austin TX.
2. The Protocol: Effective Fungal Acne Treatment at Home
You don’t always need an expensive prescription to win this battle. In 2026, “Bio-intelligent” routines are all about starving the yeast while soothing the skin. Here is your fungal acne treatment at home blueprint:
The “5-5-2” Antifungal Mask (Steps & Timing)
This is the most famous “hack” that dermatologists actually recommend in 2026 for a budget-friendly fungal acne treatment at home.
- The Product: Use an anti-dandruff shampoo containing 2% Ketoconazole (like Nizoral).
- The Application: Apply a thin layer to the affected area before your shower.
- The Timing: Leave for exactly 5 minutes.
- The Frequency: Do this 2 times a week for 4 weeks.
- Pros: Highly effective at killing yeast on contact.
- Cons: Can be drying; must be followed by a fungal-safe moisturizer.
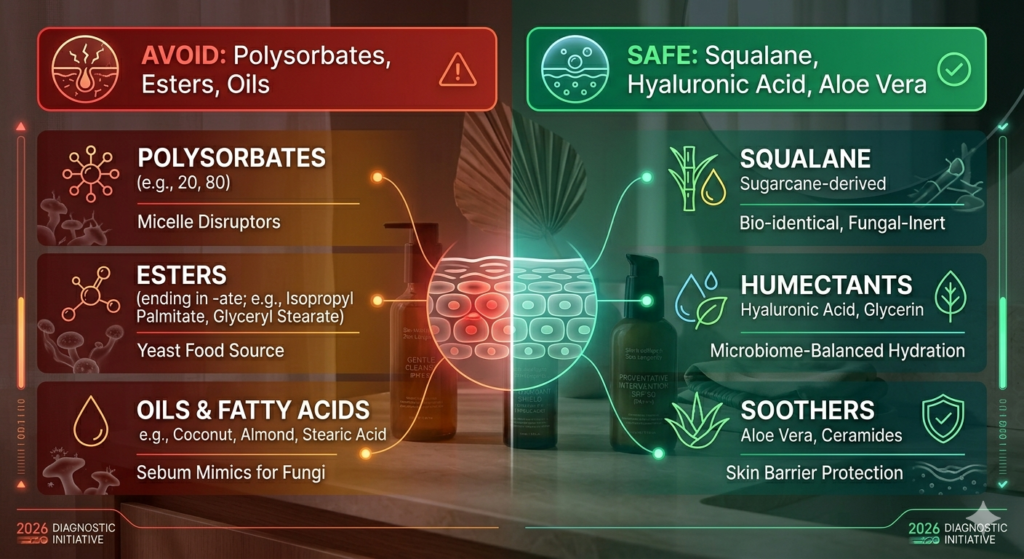
The “Red List” Ingredient Audit
Yeast feeds on specific fatty acids and oils. To clear your skin, you must audit your cabinet for:
- Avoid Oils: Coconut, Olive, and Almond oils are “yeast food.”
- Avoid Esters: Anything ending in “-ate” (like Isopropyl Palmitate).
- The 2026 Savior: Sugarcane-derived Squalane (not Squalene) is the only oil-like substance that is 100% safe for fungal acne treatment. It mimics your natural sebum without fueling the yeast.
3. Comparison Table: Fungal vs. Bacterial Ac
| Feature | Fungal Acne (Malassezia) | Bacterial Acne (Vulgaris) |
| Primary Cause | Yeast Overgrowth | Bacteria (C. acnes) |
| Common Sensation | Itchy / Prickly / Crawling | Sore / Painful / Thumping |
| Appearance | Uniform, small red bumps | Varied (Blackheads, Cystic) |
| Best Treatment | Antifungals (Ketoconazole) | Antibacterials (BHA / BP) |
| Aggravator | Humidity (70%+) & Oils | Hormones & Clogged Pores |
4. 2026 Lifestyle Pro-Tips for Skin Longevity
- The “Post-Gym 15-Minute Rule”: Sweat raises your skin’s pH, making it a playground for yeast. Use a pH 5.5 balanced micellar water within 15 minutes of finishing your workout if you can’t shower immediately.
- Fabric Longevity: Move away from tight polyester. In 2026, Bamboo and Zinc-infused cotton are the go-to fabrics for preventing “Bacne” because Zinc naturally inhibits fungal growth.
- The Hairline Guard: Your hair products often contain oils that “leak” onto your forehead. Wash your hair leaning forward to prevent conditioner from sitting on your skin.
5. FAQ: Navigating Your Treatment Journey
Q: Can I use Salicylic Acid (BHA) with fungal acne?
- A: Yes, but it won’t cure it alone. BHA helps clear dead skin cells (which yeast hides under), making your fungal acne treatment much more effective. Think of BHA as the “door opener” and the antifungal as the “fixer.”
Q: Why did my skin flare up after taking antibiotics?
- A: Antibiotics kill the “good” bacteria that keep yeast in check. This “microbiome dysbiosis” is responsible for 40% of adult fungal acne flares in 2026.
Q: How long until I see a real difference?
- A: With a consistent fungal acne treatment at home, most people see a 50% reduction in bumps within 14 days.
Conclusion: A Gentle Path to Balance
Battling fungal acne is a journey of balance, not a war of attrition. By switching to a fungal acne treatment that respects your unique microbiome, you are investing in long-term skin longevity rather than a quick, harsh fix.
My gentle suggestion? Start with the “Moisturizer Audit” tonight. Swap your oil-based cream for a 100% fungal-safe gel for 14 days and watch your skin finally breathe.
